IVF—what is it?
When the sperm and ovum from the husband and wife have been removed, in vitro fertilization is an assisted reproductive procedure used in an embryo laboratory. After fertilization and conception, the well-formed embryo will be put into the uterus to begin gestation.

The process of in vitro fertilization.
In vitro fertilization (IVF) typically commences on the 21st day of the previous menstrual cycle. At this point, the wife initiates gonadotropin-releasing hormone analog (GnRHa) to prevent hypothalamic stimulation to the pituitary gland, which ceases gonad-stimulating hormone production. After confirming a regular menstrual cycle, the wife’s ovary is stimulated with ovulation stimulants for 14-18 days to encourage the growth of additional ovarian follicles. During this period, blood tests are conducted to ascertain variations in the numerical value of estrogen levels, which are used to pinpoint the optimal window for oocyte pick-up. Additionally, an ultrasonic detector is utilized to monitor the growth of ovarian follicles.
The primordial oocyte is the smallest ovarian follicle in a woman’s ovary, measuring only 0.1 to 0.2 millimeters in diameter. The follicle’s growth is influenced by follicle-stimulating hormone (FSH). During the initial stage of menses FSH, the diameter of the ovarian follicle is merely around 5 millimeters. However, it continues to grow until it reaches a size of 8 millimeters, at which point the production of estrogen begins to increase. When the follicle attains a size of 15 millimeters, the secretion of estrogen rises significantly. The pituitary gland releases luteinizing hormone (LH) due to the high estrogen levels, causing the attenuation of partial tissue on the follicle’s surface to hasten. To complete all necessary arrangements, the patient must be reminded to obtain the human chorionic gonadotropin (HCG) injection 36 hours before egg collection.
On the day of egg collection, a transvaginal ultrasound will be employed to guide the egg retrieval process. Subsequently, the ovarian follicular fluid will be promptly transferred to the laboratory, where the ovum will be filtered and placed into a fresh Petri dish. Following this, the ovum will be combined with the semen provided by the husband and washed and percolated for 2 to 5 days until the zygote matures into a viable embryo suitable for implantation in the wife’s uterus. After ovulation, luteinizing hormone (LH) usually remains in the granulocytes and endometrial cells on the follicular wall. It gradually transforms into lutein cells, which secrete a large amount of progesterone (P4), facilitating implantation.
Separate the viable sperm from the egg and extract it from the wife’s ovary. Conduct the in vitro fertilization process by fertilizing the ovum in a petri dish for several days. Select the most suitable embryo and implant it into the uterus.


Incubation for embryos
Each incubator has a separate pipeline to feed high purity (9.999%) low oxygen (triple gas) to speed up embryo cleavage in order to generate the optimal culture environment.
Low-oxygen cultivation
The oviduct of animals contains about 5% oxygen, according to earlier studies. As a result, we add 5% oxygen to the culture environment.
Low-oxygen culture techniques
According to recent studies, the womb’s oxygen content is 1.4%, even lower than the oviduct.
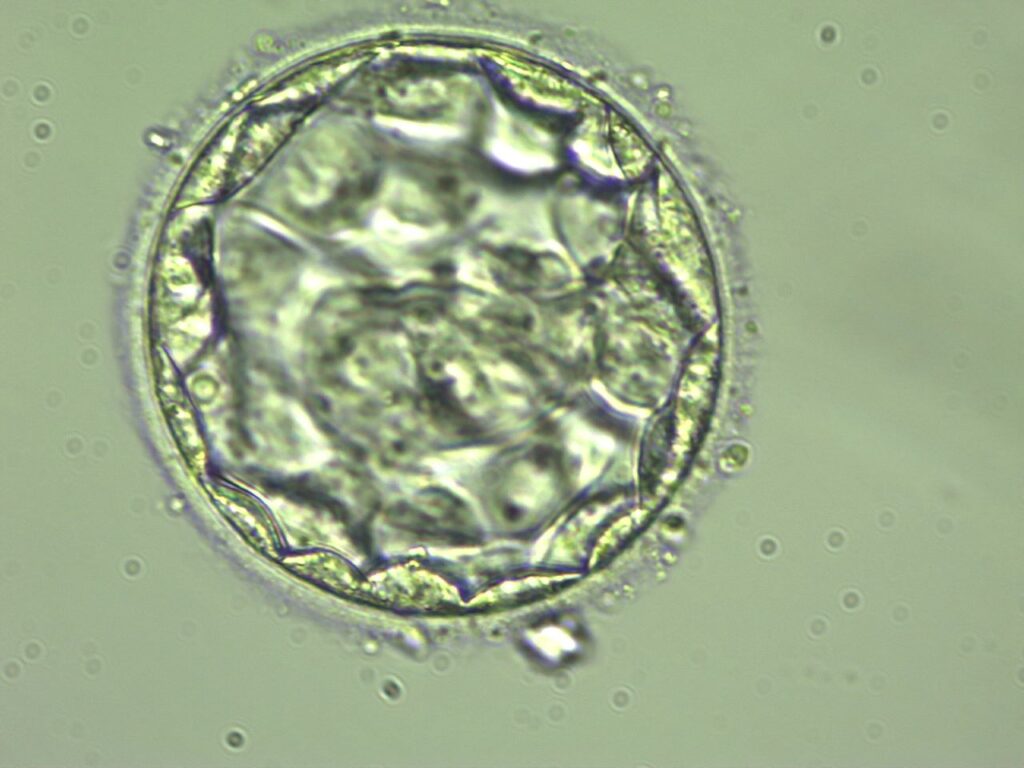
The development of the embryo may be aided by a very low-oxygen environment. Blastocyst creation is more likely, and implantation and pregnancy rates are rising. Thus, embryologists will use ultra-low oxygen culturing technology by supplying 2% oxygen to patients with poor embryo growth in order to improve embryo development.
